- 78-year-old man was admitted to hospital with a 2 week history of progressive confusion and unsteadiness.
- His medical history included parkinsonism and a metallic mitral valve replacement.
- On examination his GCS was 14/15 (E4, V4, M6) with left-sided weakness.
- He was taking warfarin, and the INR was 3.8.
Progressive confusion and gait disturbance with a left hemiparesis point to a right hemisphere lesion.
The differential diagnosis includes:
- cerebral stroke (ischemic/hemorrhagic)
- subdural hematoma,
- neoplastic lesion.
The time course of the symptoms is central to distinguishing them:
- Acute onset: intracerebral hemorrhage or stroke typically presents with sudden-onset symptoms
- Progressive onset: progressive symptoms suggest a
slowly enlarging mass such as a tumour or chronic subdural hematoma.
Head CT was performed. Describe the findings in the CT head.
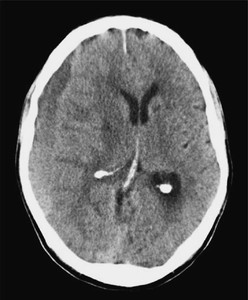
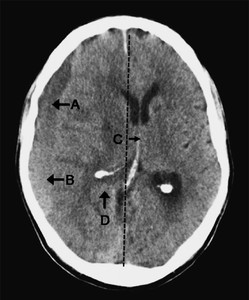
- Extra-axial crescent shaped fluid collection over the right cerebral convexity indicating a chronic subdural hematoma
- There is layering according to density, with a hypodense fluid supernatant (A) above hyperdense thrombus or cellular precipitant (B).
- This appearance could be due to a single episode of hemorrhage or rebleeding into a
chronic collection.
- This appearance could be due to a single episode of hemorrhage or rebleeding into a
- There is midline shift (C) with obliteration of cerebral sulci and the trigone (not seen, D) on the right
What is the pathophysiology of chronic subdural hematomas?
Chronic subdural hematomas are typically caused by tearing of dural bridging veins.
Cerebral atrophy (e.g. in the elderly or in alcoholic patients) causes increased tension on these veins, predisposing them to tearing.
The trauma causing the initial bleed can be sufficiently mild to be absent from the history, even in retrospect, in over 50 % of patients.
A local inflammatory reaction follows the hemorrhage and bresults in the formation of a hematoma cavity with membranes within it. The clot liquefies over time and this collection may expand. The processes that mediate this are poorly understood, but may include recurrent microbleeds from dural capillaries and hematoma membranes, secretion of fluid from hematoma membranes, and osmotic fluid shifts into the hematoma cavity.
The initial consideration is whether the patient should be managed operatively or
conservatively. Operative management is appropriate in the presence of a neurological
deficit or severe and persistent headache. In either case the INR requires normalization
and blood tests, including serum sodium and clotting, should be performed.
Surgery should be performed as soon as possible, but the practicalities of operating
overnight require consideration if the patient presents in the middle of the night.
Surgery should be considered overnight if symptoms have progressed rapidly or if
the haematoma is large (e.g. with significant midline shift and contralateral
ventricular enlargement from encystment). However, if deterioration has occurred
over several days or weeks, it would be reasonable to wait until the morning.
The wife of the patient expresses her concern about plans for surgery. She tells you that her husband was never keen on surgery and that he would not have
liked to survive with neurological impairment. She does not want you to perform the operation.
- How would you approach this conversation and what points would you cover in the discussion?
- What is the legal position of the family’s views on a patient’s treatment?
- The subdural haematoma is evacuated with burrholes, and the patient makes a good recovery. How should his anticoagulation be managed postoperatively?
Surgery should be performed as soon as possible, but the practicalities of operating
overnight require consideration if the patient presents in the middle of the night.
Surgery should be considered overnight if symptoms have progressed rapidly or if
the haematoma is large (e.g. with significant midline shift and contralateral
ventricular enlargement from encystment). However, if deterioration has occurred
over several days or weeks, it would be reasonable to wait until the morning.
There are several options for chronic subdural haematomas. Burrhole drainage is
the most common. There are specific indications for performing a craniotomy,
such as the presence of subdural membranes and recurrent episodes (see ‘Surgery
for chronic subdural haematomas ’, p. 8 and ‘Varieties of chronic subdural
haematomas’ , p. 9).
7. What are the complications of surgery?
Seizures, intracranial haematoma, pneumocephalus, and infection (including subdural
empyema). Patients should also be advised of the risk of recurrence (up to
30 % ) and risk to life with a general anaesthetic, especially in a condition affecting
an almost exclusively elderly population.